What is Bipolar Disorder?
Before I became a therapist, my understanding of bipolar disorder was shaped entirely by Hollywood. I pictured something big, scary, and unpredictable—a caricature of a person who was either "unhinged" or what I’d call a "hot mess."
However, as I encountered individuals in my life living with bipolar, my perspective was completely turned upside down. I experienced their incredible love, their boundless creativity, and a charisma so infectious it could light up a room. This was the real picture, and it was nothing like the one on screen. Sure, there were hard moments, but the good times always shone brighter.
That’s the problem with how we talk about mental health, isn't it? It’s so often stigmatized and dramatized that hearing a diagnosis can feel like a verdict. My goal is to change that narrative. I’m here to shed light on what it truly means to have bipolar disorder and share effective ways to live happily with your beautifully neurodivergent brain.
So, what exactly is Bipolar Disorder?
There are two main types: Bipolar I and Bipolar II. At its core, Bipolar I involves a combination of major depressive episodes and full manic episodes. Bipolar II, on the other hand, involves major depressive episodes and hypomania.
To receive a diagnosis of Bipolar I Disorder, a person must experience at least one manic episode. While not required for the diagnosis, many people with Bipolar I also experience hypomanic and major depressive episodes. Let's break down what each of these episodes looks like.
What is a Manic Episode?
A manic episode is a period of intense mood and energy that is a noticeable departure from a person's usual self.
Core Feeling: An abnormally upbeat, energetic, or irritable mood that lasts for at least one week (or any duration if hospitalization is needed).
Key Symptoms: You must have three or more of the following symptoms (four if the mood is only irritable):
Inflated self-esteem: Feeling overly important, powerful, or talented.
Irritability: Increase in complaints, hostile comments, or angry tirades, particularly if attempts are made to interrupt the individual.
Decreased need for sleep: Feeling rested and energetic after only a few hours of sleep.
Increased talkativeness: Talking much more and faster than usual, feeling pressured to keep talking.
Racing thoughts: Having "flight of ideas" or feeling like your thoughts are moving too fast to keep up with.
Distractibility: Being easily sidetracked by unimportant things.
Increased activity: Being unusually focused on goals (socially, at work, or sexually) or feeling agitated and unable to sit still.
Risky behavior: Getting involved in activities with a high potential for negative consequences, like spending sprees, sexual indiscretions, or foolish business investments.
Severity: The episode is severe enough to cause major problems in your life (at work, in relationships) or requires hospitalization to keep you or others safe.
Cause: The symptoms are not caused by substance use (like drugs or alcohol) or another medical condition.
What is a Hypomanic Episode?
Think of a hypomanic episode as a less severe version of a manic episode. The symptoms are similar, but the impact is different.
Core Feeling: An elevated or irritable mood and increased energy that lasts for at least four consecutive days.
Key Symptoms: The same list of symptoms as a manic episode (inflated self-esteem, less need for sleep, etc.).
Severity: This is the key difference. A hypomanic episode is not severe enough to cause major impairment in your life or require hospitalization. However, the change in your mood and functioning is still noticeable to others.
Cause: Like mania, the symptoms are not caused by substance use or another medical condition.
What is a Major Depressive Episode?
This is the "low" pole of bipolar disorder, characterized by a persistent feeling of sadness or a loss of interest in the outside world.
Core Feeling: A depressed mood or a loss of interest/pleasure in activities for at least two weeks.
Key Symptoms: You must have five or more of the following symptoms:
Feeling sad, empty, or hopeless.
Losing interest or pleasure in things you once enjoyed.
Significant changes in weight or appetite.
Sleeping too much or too little.
Feeling physically sped up (agitated) or slowed down.
Constant fatigue or loss of energy.
Feelings of worthlessness or excessive guilt.
Trouble concentrating or making decisions.
Thoughts of death or suicide.
Severity: The symptoms are significant enough to cause distress and interfere with your daily life.
Cause: The episode is not caused by substance use or another medical condition.
Treatment of Bipolar Disorder
Living with bipolar disorder means navigating a unique journey with your mind. While it has its challenges, think of it less as a life sentence and more as learning the specific operating manual for your brain. With the right toolkit of treatments and coping strategies, you can lead a happy, fulfilling, and stable life.
Building a strong foundation is key. This usually involves a combination of medication and therapy, tailored specifically to you by a healthcare professional.
Medication
Medication is often the first step in getting mood episodes under control. It’s not about changing who you are; it’s about creating a stable baseline so you can thrive. Common types include:
Mood Stabilizers: This is the cornerstone of treatment. Medications like lamotrigine are highly effective at controlling manic episodes and preventing the recurrence of both manic and depressive episodes.
Atypical Antipsychotics: These can be used to manage acute mania or depression and are also valuable for long-term mood stabilization.
Antidepressants: Antidepressants can be a tricky part of treatment because they risk triggering mania. That's why they're almost always used in combination with a mood stabilizer. This is also a key reason for misdiagnosis—many people are first treated for depression with SSRIs, which prove ineffective because the underlying issue is bipolar disorder.
Key takeaway: Finding the right medication or combination can take time. Open communication with your doctor is crucial to manage side effects and find what works best for you.
Therapy
Therapy is where you build the skills to understand and navigate your world. It's a vital part of long-term wellness.
Cognitive Behavioral Therapy (CBT): This therapy helps you identify and reframe negative thought patterns and behaviors that can trigger or worsen mood episodes. It’s like learning to become your own emotional detective.
Dialectical Behavior Therapy (DBT): DBT is fantastic for managing intense emotions. It teaches practical skills in four key areas: mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness (managing relationships).
Interpersonal and Social Rhythm Therapy (IPSRT): This therapy focuses on the importance of routine. By stabilizing your daily rhythms—especially sleep, diet, and social interaction—you can help stabilize your moods.
Lifestyle & Coping: Your Daily Toolkit
Beyond professional treatment, your daily habits and coping skills have a massive impact on your well-being. This is where you take active control.
Your brain loves predictability. A consistent daily routine is one of the most powerful tools for managing bipolar disorder.
Sleep is Sacred: Aim for 7-9 hours of sleep per night. Go to bed and wake up around the same time every day—yes, even on weekends! Poor sleep is a major trigger for mania.
Consistent Mealtimes: Eating at regular intervals helps stabilize your energy and mood.
Schedule Your Day: Knowing what to expect reduces stress and creates a sense of control.
Move Your Body & Nourish Your Brain
The connection between your body and mind is undeniable.
Exercise Regularly: Physical activity is a natural mood booster. Aim for 30 minutes of moderate exercise (like a brisk walk, yoga, or swimming) most days. It helps fight depression and anxiety.
Eat a Brain-Healthy Diet: Focus on whole foods rich in omega-3 fatty acids (like salmon and flaxseeds), lean proteins, and complex carbohydrates. Try to limit sugar, caffeine, and processed foods, which can cause energy spikes and crashes that affect your mood.
Avoid Alcohol and Drugs: These substances can interfere with your medication and are known to trigger or worsen mood episodes.
Develop Healthy Coping Mechanisms
When you feel a mood shift starting, having a plan is everything.
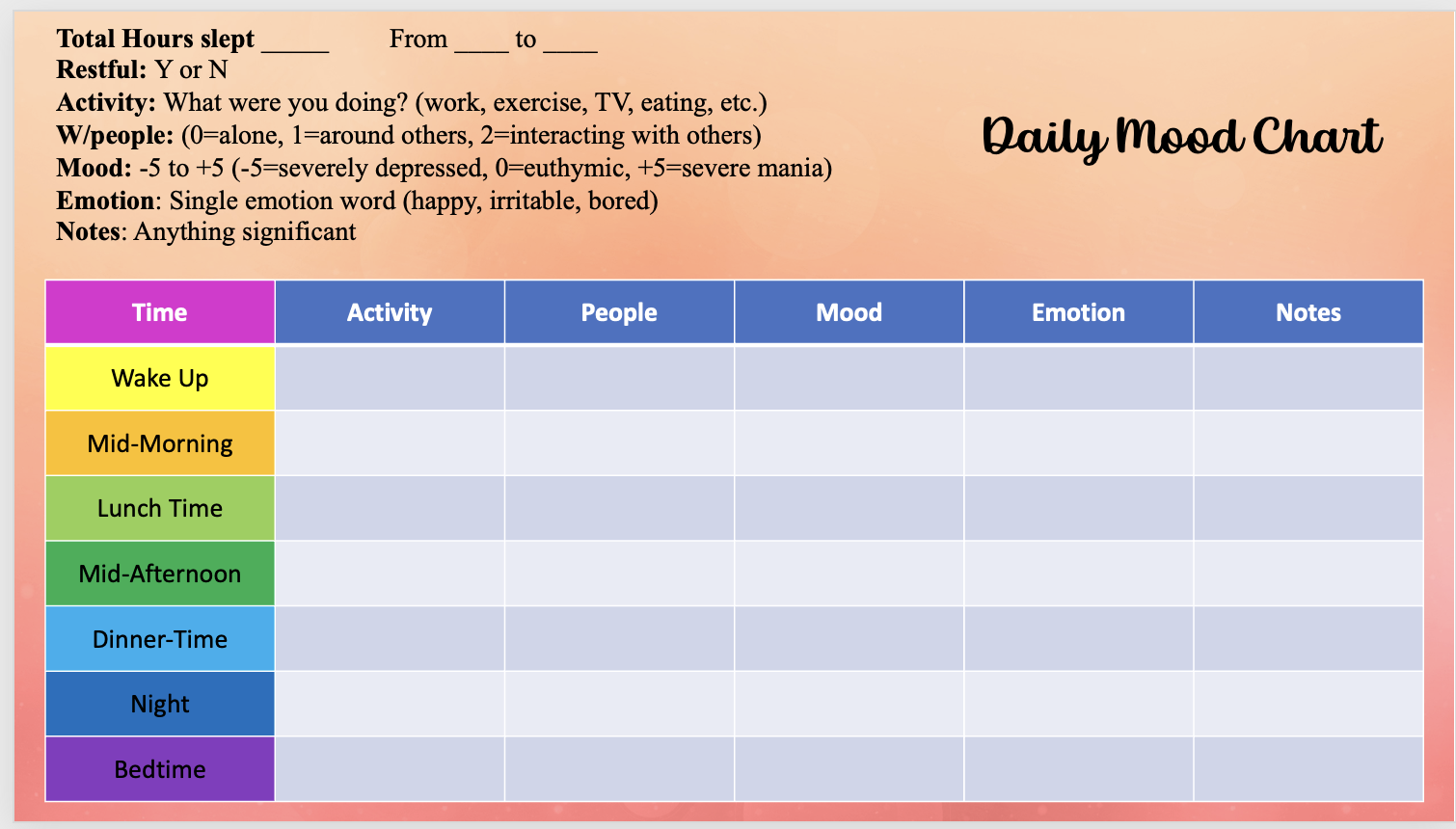
Track Your Moods: Use a journal or an app (like eMoods) to log your daily mood, sleep, and activities. Over time, you'll start to recognize your personal triggers and the early warning signs of an upcoming episode.
Practice Mindfulness & Meditation: Mindfulness helps you observe your thoughts and feelings without judgment. Even 5-10 minutes of daily meditation can reduce stress and help you feel more grounded.
Stress Management: Identify your stressors and find healthy ways to cope. This could be deep breathing exercises, spending time in nature, listening to calming music, or diving into a hobby.
Journaling: Writing down your thoughts is a powerful way to process emotions, release pent-up feelings, and gain clarity.
Understanding your triggers is key. A simple way to do this is by tracking your daily moods and activities. Use this chart or a journal to log how you feel, what you did, and your energy levels. Look for patterns—this will give you powerful insights into how your bipolar symptoms uniquely affect you, helping you stay one step ahead.
Build Your Support System
You don't have to do this alone. A strong support network is essential.
Lean on Trusted People: Be open with close friends and family who are supportive and understanding. Let them know what your warning signs are and how they can help during a difficult time.
Join a Support Group: Connecting with others who have similar experiences can be incredibly validating. Organizations like the National Alliance on Mental Illness (NAMI) and the Depression and Bipolar Support Alliance (DBSA) offer free peer-led groups.
Living with bipolar disorder is a journey of learning and adapting, but you don't have to walk it alone. By pairing professional treatment with a personalized toolkit of daily strategies, you can build a life full of joy, creativity, and connection. If you're ready for support, the clinicians at Snow Lake Counseling are here to help. Reach out to schedule your free consultation today and let us help you find the perfect therapeutic fit.